Written By: Dr. Jenna Henderson
The views expressed in this article are not The Hopes or its sponsor Kibow® Biotech, they are those of the author. This article is not intended to be viewed as medical advice. Please check with your health care provider before starting to take any herbal supplements.
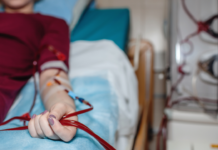
My nephrologist broached the subject of home hemodialysis and thought I’d be a good candidate for it. I’d watched the nurses working for years. These machines were complicated, and when things went wrong these professional nurses worked together to troubleshoot. Operating one of these machines on my own? Inserting my own needles? That’s not going to happen, I told my nephrologist. The last thing I needed after a long day’s work was to figure out how to clean my own blood. Why not just show up in the clinic with a professional standing by and the machine ready to go?
There are some things in life I don’t mind leaving to the experts. If I really wanted to learn the inner workings of my car, I could, but I’m actually quite happy to leave this task to my mechanic. He has proven himself trustworthy and competent, so I go along with his recommendations. And for most of my years on dialysis, this was my attitude toward treatment. The dialysis nurses know what they’re doing, so I was fine leaving my dialysis sessions in their hands.
But things were not fine. After 2 decades without my native kidneys working, cracks were starting to show. Recurrent FSGS caused me to lose my transplant, and the odds were overwhelming that FSGS would attack any new transplant. Some patients go down the road of multiple kidney transplants, but I decided to not force the situation and go through more surgery only to lose a new kidney. So until something better came along, the dialysis clinic would suffice. But would it?
My nephrologist told me of better survival rates of patients who do more frequent dialysis. Home dialysis sessions were shorter but 5 to 6 times a week rather than 3 times a week. This means that there is less time between sessions for uremic toxins to build up. To convince me he ordered that I do treatments in-center 6 days a week. I was annoyed to say the least, but I complied. Okay, for a short time I’ll agree to try it your way.
Much to my surprise I did feel better. Doing treatment 3 days a week, my energy level just wasn’t that good. During the work day I took 15 minute breaks here and there to put my feet up when fatigue took over. At home I needed to pace myself doing simple chores before feeling too tired. This became normal. But now I could feel the difference. I could work 8 hours straight without a break. I had been concerned about the extra time in clinic disrupting the rest of my life, but it seemed I actually got more done in my free time. The frequent sessions really did make me feel better. And certainly cleaner blood must help long term survival.
Doing more frequent sessions came with plenty of benefits. My fluid gains between sessions were usually around 1.0 kilogram. When I did treatment 3 times a week 2.5 kilograms was the norm and over the weekend it could be considerably more if I ate saltier food in a restaurant. With less fluid to remove, treatment was more comfortable. There were no sudden drops in blood pressure and no muscle cramps. Controlling potassium and phosphorus also came much easier with frequent dialysis. That month with 6 day a week sessions, my monthly labs looked great.
I agreed to continue to come into the center 6 times a week. Oh, no it doesn’t work that way. Medicare won’t pay for more than 3 session per week. This was just a trial run. If you want the benefits of frequent dialysis, you have to do it at home. I relented, okay I’ll give home hemodialysis a try.
I was trained with the “Baby K” machine, which is the most difficult to use, but cleans the blood very well. And yes, it’s hard. Learning how to operate a home hemo machine is like learning to drive a car for the first time. It’s full of complicated rules and if you skip even one step, you can be in big trouble. The 2 months of training with a nurse was literally blood, sweat, and tears. Some people thought it would be easier for me, having had some training in a medical field, but when the blood pump stops and the machine goes into alarm, it doesn’t matter how well you did in Organic Chemistry; it’s a frightening ordeal.
My first treatment at home without the training nurse was a nightmare. Pretty much everything that could go wrong did. I was ready to give the whole thing up. Then a family member said, “Why don’t you give up your business and go on Medicaid?” What! That was unthinkable. I made up my mind, I’m going to do this no matter what it takes.
And persistence paid off. It did get easier. After you see the same alarm a few times, it’s not so intimidating. Okay, I can troubleshoot. The biggest challenge was learning not to panic. Like anything in life, things go wrong. I learned to appreciate just how often treatment went right with no alarms, rather than get upset every time the machine had trouble.
It also helped to appreciate just how dedicated the home hemodialysis team was. I could call the nurse or a technician at odd hours when I needed help. When the machine needed repair, the tech drove right out and made sure I never missed a treatment. When my town had a water contamination crisis, emergency supplies of dialysate fluid were on my doorstep within 24 hours. If they put forth this much effort to make my home treatments work, I could make my best effort too.
Inserting needles is still not easy. The needle goes in part way and then there’s resistance. Even when you get the angle of insertion right, it can hurt pushing the needle. The nurse explained that if there was no resistance, you’d bleed out all the time. Resistance is necessary. To move forward requires you to keep pushing, even when it gets uncomfortable.
As my comfort level grew, I started to appreciate the benefits of home treatment even more. Once you work past the challenges, there is a new freedom. The first time a major snowstorm hit, I didn’t have to worry about fighting the icy roads to get to the clinic. I realized why very few patients who do home hemodialysis go back to doing it in-center. Setting my own treatment time didn’t seem like a big deal at first, but this new flexibility began to make life much easier. Do I want to take off Christmas Eve or Christmas day? It was completely my decision. Can I do treatment early in the morning then take a flight in the evening? Sure that’s easy and I don’t need permission.
Treatment itself was more comfortable at home. I could arrange the dialysis space with a nice easy chair and place for my laptop. Best of all, I could set the thermostat to anything I wanted. Dialysis session were often uncomfortable just because I was cold. With the temperature in the clinic set to 69/70o and blood outside the body, even with a good blanket, I felt cold. It’s interesting how the three hour session seems to go much faster when you’re physically more at ease.
Home hemodialysis does require a lot of space in your home. It’s not just the dedicated area where the treatment takes place, but storage space for supplies. It’s a lot of supplies. It’s something I couldn’t have done living in a small apartment in graduate school. It also requires plumbing modifications to the water supply. I’m fortunate now that I do live in a house that lends itself well to the process.
I’d like to say that I missed the comradery of the other patients, but that wasn’t the case. In the waiting room of the clinic there were polite hellos and nods. Sometimes the patients would complain about a particular worker, but for the most part patients bore their own problems stoically and didn’t say much at all. Shared hardships often draw people together, but sometimes they don’t. Actual conversations with other dialysis patients mostly took place online. On Facebook other dialysis patients were eager and enthusiastic to learn about how natural medicine could help them. Telling the patient in the chair next to me that some natural supplements can help dialysis patients, was generally met with blank stares and awkward pauses.
Looking back on the dialysis experience, I remember not working in 1998 when I first started dialysis. Then I went back to work part-time, then full-time. By 2009 I was running my own business. Each time I progressed forward it was a hard push but worth it. Gaining a sense of independence and self-reliance became more important over time. Moving to home hemodialysis in 2016 now seems like a critical step toward that goal.
With survival rates comparable to a kidney transplant, home hemodialysis has been a good decision. It’s a relief to not have the side-effects of the transplant medications. It’s also a relief to not be waiting for a transplant with a sense of desperation. Taking charge of dialysis is within my control. Waiting for someone else’s kidney is not.
I’ve moved on to the NextStage home hemodialysis machine. Although my clearance is not quite as good as it was with the “Baby K”, the process is a lot easier. NextStage also comes with an iPad that communicates with the dialysis machine and transmits to the dialysis nurses. This is a lot easier than filling out paper flow sheets to submit. My dialysis experience has certainly been a lot easier than my cousin’s in the 80s, and dialysis in the 80s was much better than when it first started in the 40s. Lots of hard work was necessary for every medical innovation that’s made my life easier.
Home hemodialysis is still a challenge. There are days when I have to remind myself why I’m doing it. There’s always a moment of anxiety when the machine first powers up. It’s like the take off of a plane and no matter how many times you do it, there’s that initial uneasiness. But then the caution light goes away, you relax and everything is going to be okay.
Sponsor: Kibow® Biotech 
About the author, Dr. Jenna Henderson